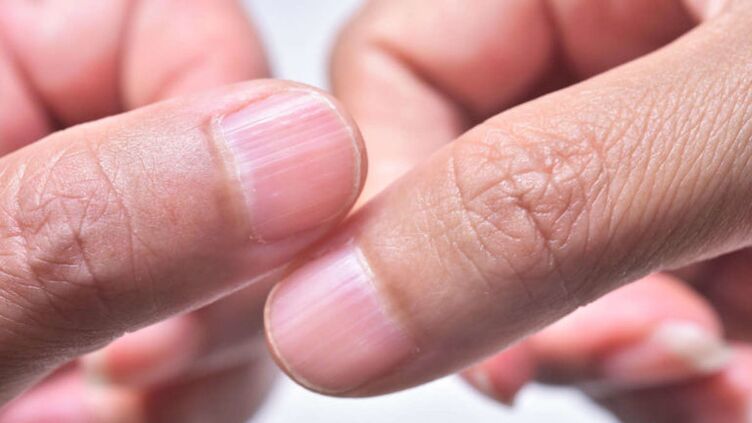
Nail psoriasis is a typical form of psoriasis in which the nails on the hands and / or feet are affected. Doctors call this disease psoriatic onychodystrophy (from the Greek.onychos- chicken,disease- violation,trophy- food).
From this article, you will learn about the causes of the development of nail psoriasis, its symptoms, which do not always indicate an accurate diagnosis, as well as dangerous misconceptions about this form of the disease.
Note.There are many pictures in the article that can scare the unprepared reader.
Where do nails grow from?
To understand the problem of nail psoriasis, it is important to understand how the so -called nail tools work.
Nails have two functions: functional and aesthetic. First, the nail protects the fingertips from damage, improves accuracy and sensitivity when working with small objects, it can be a weapon of attack or defense, and finally, with the help of our nails itch. Second, the aesthetic or cosmetic function of the nails is also important, especially for women.
Nails are formed from the outer layer of the skin - the epidermis. Nail tools include:
- nail plate - directly the nail itself,
- matrix - it produces a nail plate,
- the nail hole, or lunula, is the only visible part of the matrix, this is the white moon-shaped area at the base of the nail plate,
- eponychium - a nail roller that protects the matrix from above from damage,
- nail bed - located under the nail plate and responsible for attaching to the phalanx of the fingernail,
- hyponychium - the transition zone between the nail bed and the skin of the fingertips.
Causes and mechanisms of development of nail psoriasis
In its course - with periodic increases and decreases - psoriasis on the nails resembles a form of vulgar disease.
It is believed that nail psoriasis develops for the same reason and in the same pattern as a common psoriatic eruption. Among these reasons, external and internal factors are distinguished.
The main intrinsic factor is genetic predisposition. External causes are numerous and include, such as injuries, poor diet, intoxication (alcohol and tobacco), infections, and certain medications.
The standard mechanism of development of nail psoriasis under the influence of these causes can be briefly described as follows:
- Encouraging factors, such as trauma, activate immune cells.
- Activated immune cells migrate to the nail matrix area or nail bed.
- Immune inflammation develops in this area.
- The division of skin cells is accelerated rapidly, and its maturation is disrupted.
- There are special features of psoriasis on the nails.
Also, the cause of nail psoriasis can be thought of as a result of the body’s inability to adapt to adverse environmental conditions. According to this view, the main cause of psoriasis is an evolutionary foreign habitat.
As a result, this evolutionary approach considers unhealthy diets, lack of sunlight and clean water, excessive toxins, lack of normal physical activity, sleep disturbances and chronic stress as direct causes of disease.
Nail psoriasis and psoriatic arthritis are linked
The link between nail damage and psoriatic arthritis has long been known.
Based on observations, scientists have found that psoriatic arthritis is accompanied by nail damage in nine cases out of ten.
But the mechanism of this relationship has not been fully studied. However, the authors of several studies, for example, from the Institute of Molecular Medicine in Leeds (UK), tried to explain this relationship beyond the concept of immune inflammation.
In their opinion, the fact is that the finger joint is located next to the nail and is anatomically linked to it.
Thus, microtrauma and the Kebner phenomenon that causes primary joint inflammation - psoriatic arthritis - also cause secondary pathological changes in the nearby nail.
This is why psoriatic arthritis is often associated with nail damage.
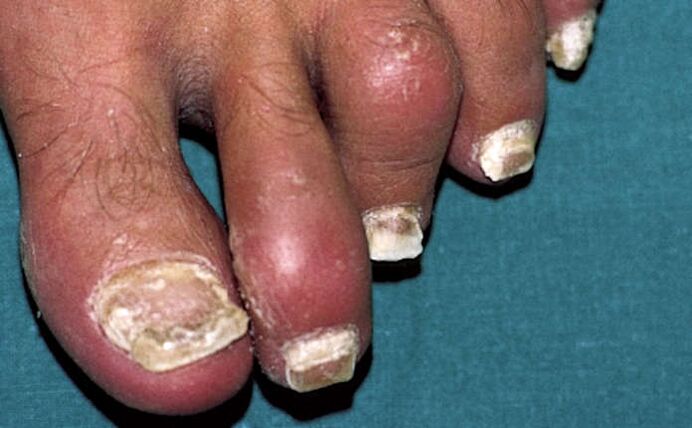
Therefore, the symptoms of nail psoriasis often indicate psoriatic arthritis.
Now let’s look at the main myths that accompany this disease, and how dangerous it is.
Myth 1: Nail psoriasis is rare.
Not really. Apparently, with psoriasis, nails very often suffer.
According to various sources, nail psoriasis occurs in the range of 6% to 82% of cases of psoriasis vulgaris. The widespread prevalence in assessing the prevalence of this pathology is explained by problems in its accounting. Medical statistics register visits to the doctor in the first place by patients with vulgar forms, and attention is given to the nails in the second place. In scientific research, cases of nail psoriasis are also usually studied in addition to the main object of interest - psoriasis with skin lesions.
However, a number of publications say that
up to 80-90% of patients with psoriasis vulgaris report recurrent nail damage.
And also that nail psoriasis occurs in 90% of patients with psoriatic arthritis and scalp psoriasis.
It should be noted that usually adults suffer from this form of the disease.
According to various sources, in children, nails are affected in about 7-37% of psoriasis cases. Unfortunately, often the manifestations of psoriasis on the nails of children are not given due attention. Parents or doctors believe that this is a variant of the norm or a result of trauma, or they do not notice it because of the mild severity of symptoms.
Myth 2: Recognizing nail psoriasis with symptoms is easy
Actually, not always. The fact is
nails can respond to a variety of diseases with just a few symptoms. Therefore, the manifestations of various diseases on the nails may look similar.
Of course, nail psoriasis can be suspected if the patient has severe symptoms of psoriasis vulgaris. However, nail lesions can be small compared to lesions on the skin and easily ignored by doctors.
Usually, the more active the psoriasis on the skin, the worse the damage to the nails.
First of all, the nails are affected.
And it is also important to know that in 5% of cases, nails may be the only early manifestation of psoriasis. That is, the classic manifestations of psoriasis on the skin may not be completely absent.
How nail psoriasis looks depends on where the pathological changes come from - in the matrix or layer of the nail.
The cause of the symptoms - the matrix or the bed - is important to consider when choosing a treatment. Therefore, it is necessary to determine it correctly.
Symptoms that come from the nail matrix are:
- thimble symptoms,
- white spots and spots (leukonychia),
- red dot in the hole,
- The nails are crumbling.
Although the cause of these symptoms is at the level of the matrix, as the nail grows, pathological changes appear in the nail plate.
The symptoms, the cause of which is in the nail bed, are:
- nail detachment (onycholysis),
- longitudinal bleeding,
- subungual hyperkeratosis,
- oil stain symptoms.
Next, we will think about each symptom separately. And let's start with the manifestations that come from the matrix.
Thimble symptoms
Thimble symptoms appear on the surface of the nail plate with holes or holes, which look like pressure on the thimble.
Such defects occur mainly on the nails, but rarely appear on the feet. As the nail grows, the hole moves from the fold of the nail to the edge of the nail plate.
Holes in nail psoriasis are usually deep, large and chaotic. They arise due to loose clustering of cells from the surface of the nail, where fission and keratinization are disrupted.
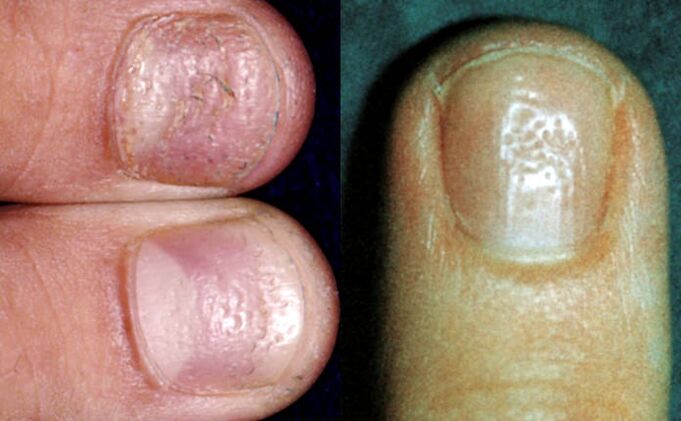
The worse the psoriasis, the more frequent the symptoms of thimbles.
However, it should be remembered that, in addition to psoriasis, holes in the nails are also characteristic of alopecia areata (alopecia), eczema, dermatitis, and can also occur, for example, with fungal infections.
Counting the number of holes on all nails will help make a correct diagnosis.
- Less than 20 - not uncommon for psoriasis,
- 20 to 60 - psoriasis can be suspected,
- more than 60 - confirm the diagnosis of psoriasis.
White spots (leukonychia)
Leukonychia is a symptom that manifests itself as white spots or spots on the nails.
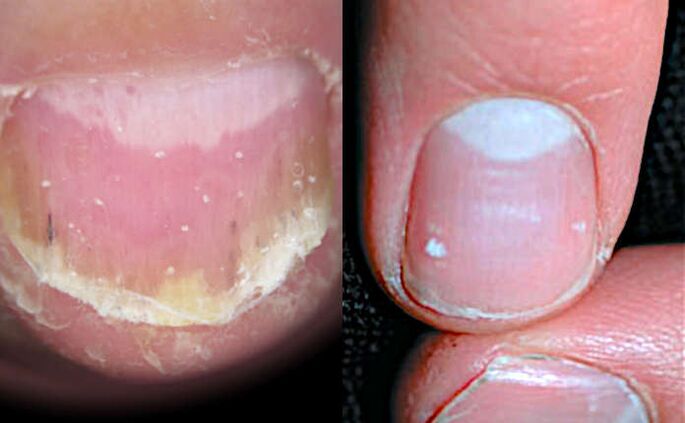
With leukonychia (from the Greek.leukós- white andonychos- nails), in contrast to superficial holes in the thimbles symptoms, cells with disturbed cleavage and keratinization are located in the thickness of the nail plate. At the same time, the surface of the nail remains smooth. And the white color of the spots arises from the reflection of light from a group of cells that are located loosely.
However, some studies show that leukonychia is so common in healthy people that it is not a symptom of psoriasis. For example, a manicure injury can cause leukonychia.
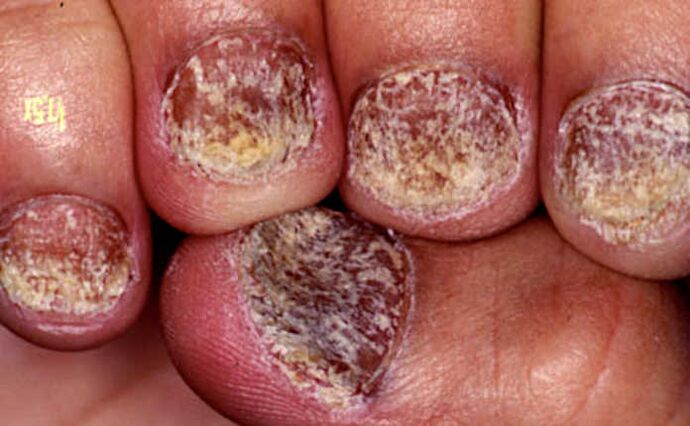
Broken nails
When the superficial hole (thimble symptoms) and the deep leukonychia zone (white spots) merge, the nail begins to crumble.
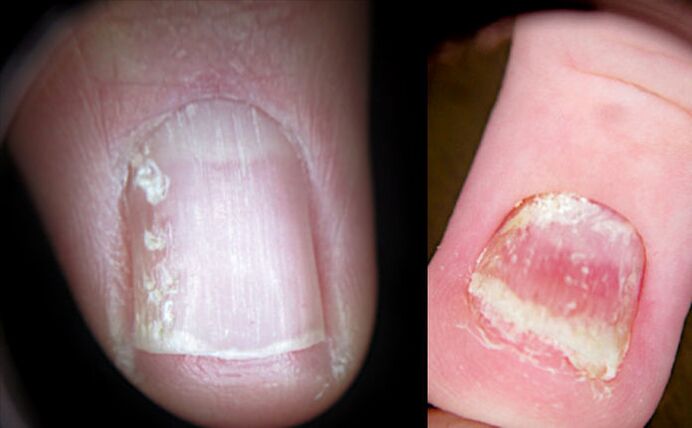
Typically, nail cracking occurs with long -term nail psoriasis.
And the stronger the inflammation of the nail matrix, the more the nail plate is destroyed. In severe cases, the nail can collapse and fall off completely.
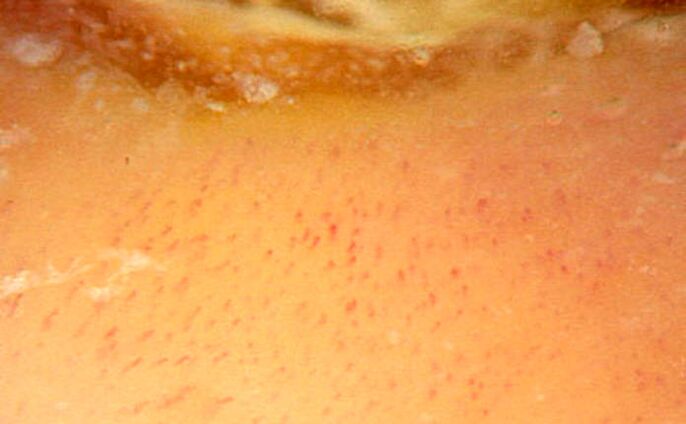
Red dot on the nail socket
Apparently, red dots in the hole area and redness generally occur due to increased blood flow to the ducts under the nail.
Also, red dots on the holes are formed due to violation of the structure of the nail plate itself: it becomes more transparent and thinner. Therefore, first, the vessel becomes more visible, and second, the thin nail plate puts less pressure on the vessel beneath it, and is more blood -filled.
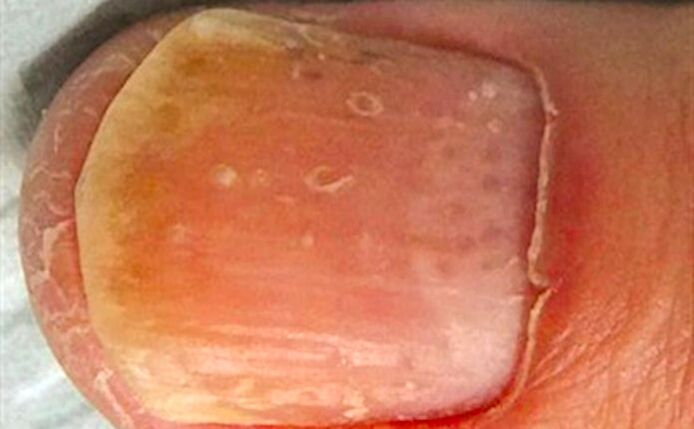
Thinning of the nail plate can also cause redness on the entire nail.
Nail removal (onycholysis)
Now let's look at the symptoms, the source of which is the nail bed.
Onycholysis is the separation of the nail plate from the bed due to the accumulation of cells under the nail with disrupted cleavage and keratinization.
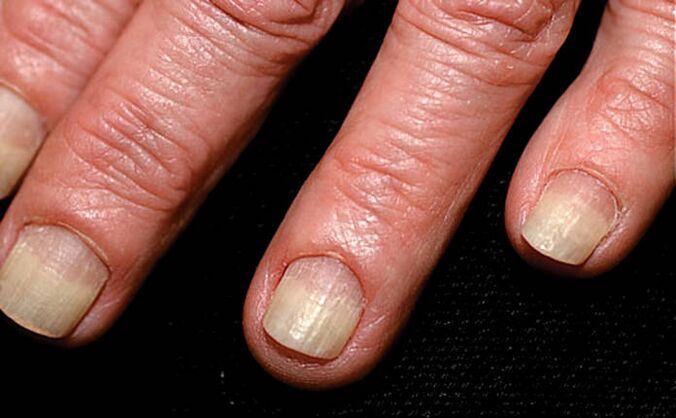
Onycholysis itself (from the Greek.onychos- And nailsλύσις- separation) is not necessarily a sign of psoriasis and can develop, for example, as a result of nail injury.
Initially, the loss of contact between the nail and the bed occurs in the zone of hyponychia - along the outer edge of the nail plate. Then onycholysis spreads towards the folds of the nail in the form of a semicircular line. The exfoliation area turns white due to the accumulation of air under the nail.
The border of redness (scientifically erythema) along the edges of onycholysis, which is usually visible on the fingers, is characteristic of psoriasis and helps make a correct diagnosis.
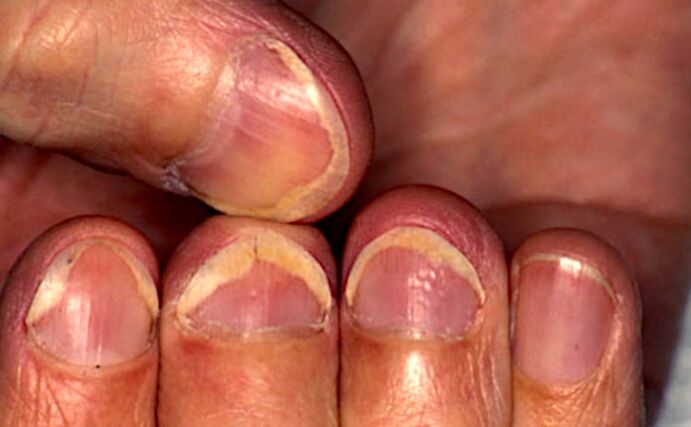
With prolonged onycholysis, the nail bed loses its properties and the new nails that grow, most likely, will not be able to attach to it normally. Therefore, even with complete renewal of the nail plate, onycholysis often occurs.
Due to the fact that onycholysis facilitates the penetration of bacteria and fungi, infections can combine. This sometimes leads to discoloration on the nails. For example, a greenish color can occur when bacteria are attachedPseudomonas aeruginosa(Pseudomonas aeruginosa) and others.
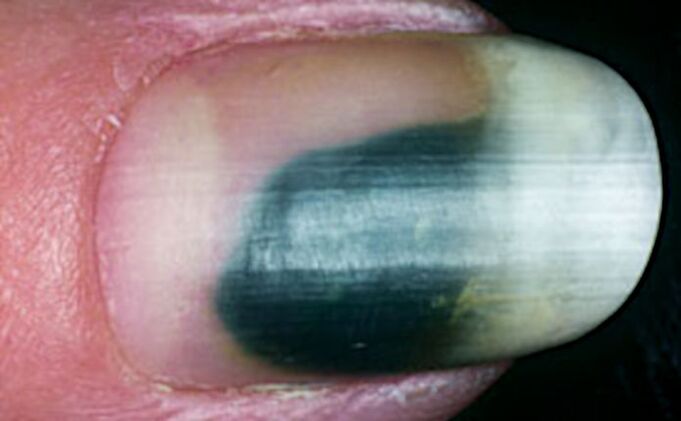
Longitudinal subungual hemorrhage
Longitudinal subungual hemorrhage occurs in the nail bed and looks like a dark red line 1-3 mm long.
Increased blood flow and edema in the inflamed area of the nail cause rupture of the capillaries, which manifest themselves in the form of such bleeding.
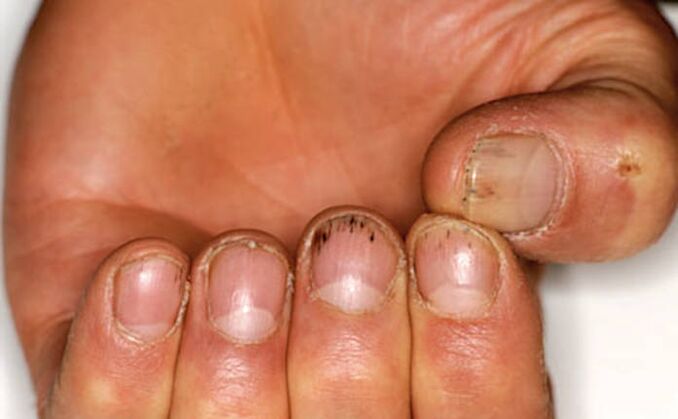
Due to the privilege of the blood supply, most bleeding occurs closer to the free edge of the nail - in the zone of hyponychia.
Subungual hyperkeratosis
Subungual hyperkeratosis is the accumulation of dead cells under the outer part of the nail plate.
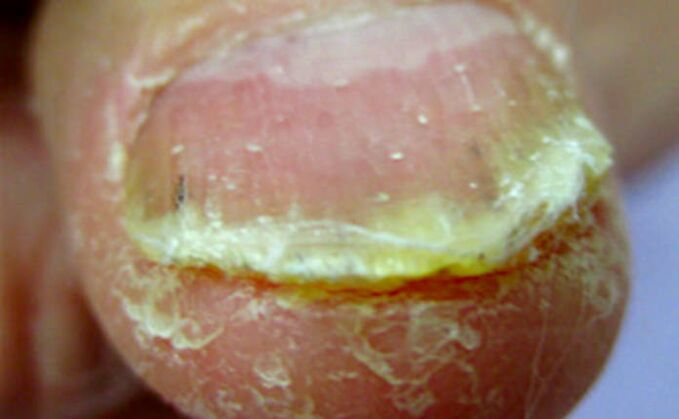
With psoriasis, subungual hyperkeratosis (from the Greek.hyper- excessively andhard- horns) are usually silvery white, but also yellow. And when the infections merge, it can be, like greenish or brown.
The higher the nail on the nail bed, the higher the activity of pathological processes.
On the fingers, subungual hyperkeratosis is usually indicated by a loose layer beneath the nail plate. On the feet, this mass is strongly soldered with thickened nails.
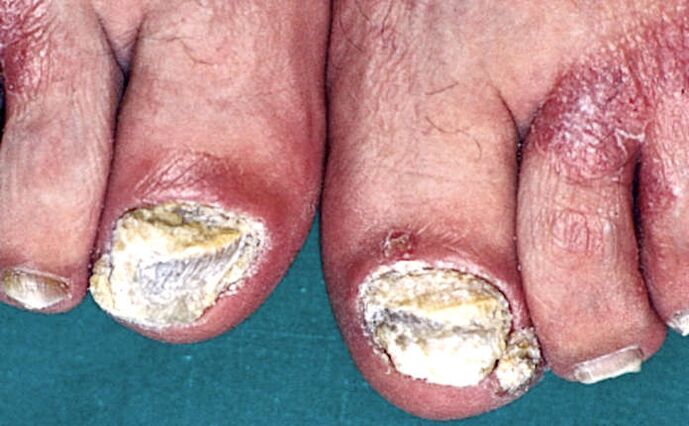
Also, psoriasis with toenail lesions is characterized by a combination of subungual hyperkeratosis with onycholysis (separation of the nails).
Symptoms of oil stains
Symptoms of oil stains appear under the nail plate on yellow-red spots (salmon).
They appear on the nail bed closer to the nail fold and move towards the edge of the nail as it grows.
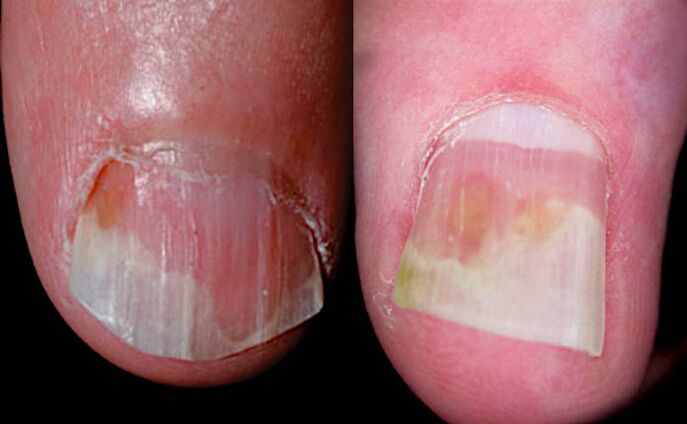
The cause of these symptoms is inflammation of the nail with capillary expansion and accumulation of cells involved in inflammation, as well as cells with impaired cleavage and keratinization.
Oil stains come in a variety of shapes and sizes. They can be found in the center of the nail and on the edges, next to the onycholysis zone.
Myth 3: nail psoriasis is just a cosmetic problem.
Actually this is not true. Although more than 90% of patients report unsightly psoriasis nails, this is not just a cosmetic problem.
According to various studies, nail psoriasis significantly reduces the quality of life of patients:
- 52% of patients also complain of pain,
- 59% - for problems in daily activities,
- 56% - for difficulties at home and
- 48% - for difficulties in the workplace.
Therefore, it is very important to make an accurate diagnosis and start treatment as early as possible, because improving the condition of the nails significantly improves the quality of life of patients with psoriasis.
Myth 4: nail psoriasis is harmless
Actually, this is not the case. Talking above about the causes of this form of the disease, we have written it
Nail psoriasis is an important symptom of psoriatic arthritis.
It is important to remember that external manifestations of arthritis may be completely absent. In this case, we can talk not only about the fact that the joints of the fingers and toes are affected, but also the joints of the spine and pelvic bones may be involved.
You can check your joints for arthritis with ultrasound (ultrasound) or magnetic resonance imaging (MRI).
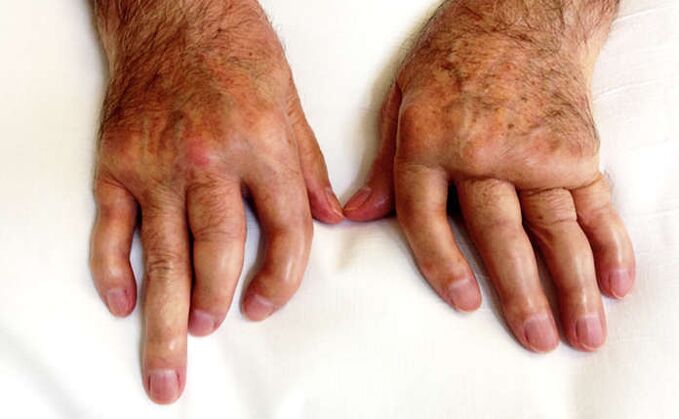
Although there are no obvious symptoms of arthritis, but there are manifestations of nail psoriasis, it is very important to ensure that all joints are in order.
And then regularly monitor the condition of the joints. Otherwise, psoriatic arthritis is easy to miss! Late diagnosis will result in late treatment and, as a consequence, irreversible joint damage and deformity.
Therefore, if the doctor has not ordered research on insurance, on the grounds of the absence of obvious signs of arthritis, you must contact the clinic yourself and undergo, for example, an ultrasound scan on a paid basis.
How to diagnose nail psoriasis
It is important to be able to recognize the many symptoms of nail psoriasis, which we have described above, because it helps determine the correct diagnosis. But because nail changes characteristic of psoriasis can occur in other diseases as well, it is difficult to immediately make an accurate diagnosis.
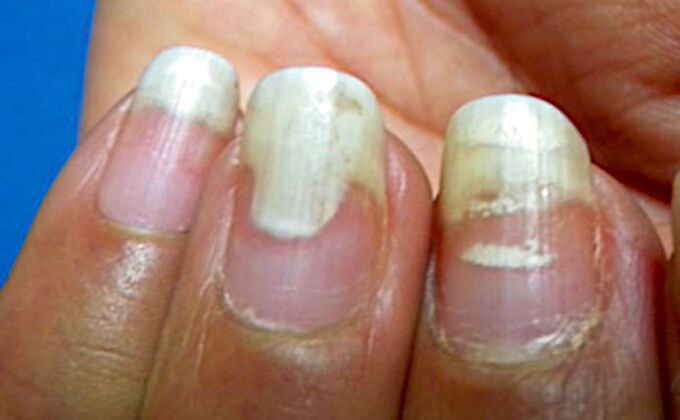
In this case, the presence of several symptoms on different nails can help in the diagnosis.
Important signs of psoriasis on the nails are:
- thimble symptoms: more than 20 holes on all fingernails indicate the possibility of psoriasis, and more than 60 holes confirm the diagnosis of psoriasis,
- nail detachment (onycholysis) with a reddish border around the edges,
- oil stains (salmon) at the base of the nail.
Difficulty in diagnosing nail psoriasis with one symptom
It is very difficult to diagnose nail psoriasis if it only shows one symptom.
For example, if it only shows onycholysis on the hands or only subungual hyperkeratosis on the arms and / or legs.
The only method to make a reliable diagnosis in isolated onycholysis (nail detachment) may be the study of hyponychia using a special microscope - a dermatoscope.
For this, a high magnification video dermatoscope was used. Please note that handheld dermatoscopes do not provide the required magnification. All that is needed is a video dermatoscope with magnification of at least 40 times. Then the features of the widening capillary loop from psoriasis become visible.
With isolated subungual hyperkeratosis, the likelihood of psoriasis is high if the accumulation of scales under the nails is whitish-silver in color, as well as if all the nails on the hands or feet are affected.
Psoriasis or nail fungus?
About 30% of patients with nail psoriasis also develop a fungal infection - onychomycosis scientifically.
Externally, hyperkeratosis and onycholysis (separation of nails) in psoriasis can resemble manifestations of fungal infections. Therefore, it is difficult to carry out differential diagnostics, that is, to identify the true cause of changes in the nail plate.
Moreover, both psoriasis and fungus can affect the same nails at the same time. Often it occurs on the toes and is a hallmark of elderly patients.
Also, with fungal infections, one or both nails on the big toe are often affected. In psoriasis, as a rule, several nails are affected at once.
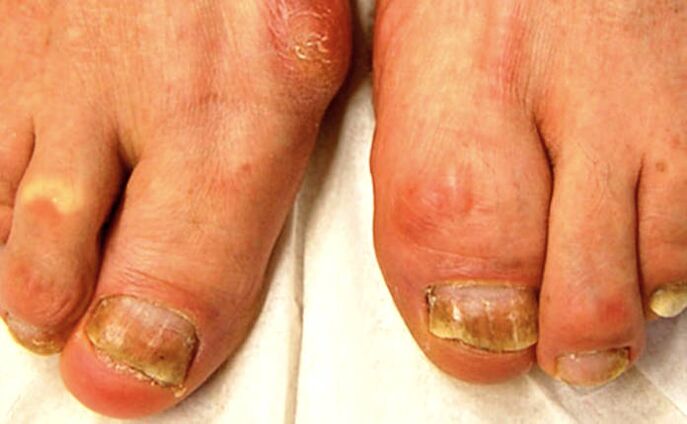
The following symptoms support psoriasis:
- oil stains and / or thimble symptoms on fingernails,
- signs of psoriasis on the scalp and / or large skin folds,
- periodic remission and exacerbation of nail damage.
In favor of onychomycosis they say:
- longitudinal path on the affected nail,
- detection of fungus during examination under an abrasion microscope treated with potassium hydroxide from the affected nail (KOH test),
- positive culture for fungi.
In general, only on the basis of external manifestations, it is impossible to completely get rid of nail infections on the nails in patients with psoriasis.
It should also be kept in mind that fungal infections can cause the Kebner phenomenon on the nails and the surrounding skin, resulting in symptoms of psoriasis. Therefore
it is useful to go to a mycologist and do a test for fungus and, if found, start antifungal therapy.
Important findings and what needs to be done
Let’s summarize important information about nail psoriasis and its symptoms.
Diagnostic features:
- Nail psoriasis is very common but often goes away.
- The manifestations of nail psoriasis can be minor, so that experts also often do not pay attention to it.
- In 5% of cases, nail damage may be the only early symptom of psoriasis.
- The manifestations of different diseases on the nails may look similar, which also complicates the diagnosis.
The main manifestations of nail psoriasis:
- thimble symptoms - holes in the nails,
- white dot,
- The nails are crumbling
- red dot in the hole area,
- nail detachment,
- longitudinal subungual hemorrhage,
- subungual hyperkeratosis - loose clusters under the nail,
- oil stain symptoms.
Psoriasis and fungi:
- Often, nail psoriasis is accompanied by a fungal infection.
- To exclude it strictly, it is necessary to contact a mycologist and conduct additional research.
Nail psoriasis and psoriatic arthritis:
- Nail psoriasis is a companion of psoriatic arthritis.
- It is important to detect pathological changes in the joint as early as possible in order to begin treatment in a timely manner and avoid complications and irreversible deformities.
- Although there are no symptoms of external arthritis, but nail psoriasis is detected, should undergo joint examination using ultrasound or MRI.























